
CRANE Report 2021
In partnership with The CRANE Database, CLAPA is pleased to publish the findings of their 2021 summary report for patients, parents and carers below.
Since 2012, these reports have given us a great deal of insight into cleft lip and palate in the UK, and have helped clinicians push for higher standards across the board.
As part of the UK cleft community, we hope you enjoy reading about the latest statistics CRANE have collected on children born (or registered with the database) between 1st January 2000 – 31st December 2020.
Please note: These figures are for births in England, Wales and Northern Ireland only. Figures from Scotland are collected slightly differently, though CRANE hopes to produce reports in the future that contain these as well.
Download the 2021 Report (PDF)
Contents
- What is a Cleft Lip and/or Palate?
- What is the CRANE Database?
- What other information does CRANE collect and use?
- What do we know about children born with a cleft and registered in CRANE between 2000-2020?
- What do we know about children born between 2017-2019 with a cleft?
- What do we know about 5-year-old children (born 2011-13) with a cleft?
- What we understand from our most recent review of audit and health information
- Find out more
- Glossary
What is a Cleft Lip and/or Palate?

A cleft is a gap in the upper lip, the roof of the mouth (palate), or sometimes both. This is a common birth condition that can affect a number of functions including feeding, speech and hearing. Children’s dental and psychosocial health may also be affected (see the Glossary for more information on psychosocial health).
The cleft can involve part or all of the lip and/or palate and there are 4 types of cleft: Cleft palate (CP), cleft lip (CL), one-sided clefts known as a unilateral cleft lip and palate (UCLP) and clefts that affect both sides of the lip and palate known as bilateral cleft lip and palate (BCLP) (see the Glossary for more information on clefts).
Surgery usually takes place in the first year of life. Children may have further surgery to address function or appearance as they grow. Other non-surgical help and support such as speech therapy, hearing support and psychological support may also be needed by some children.
What is the CRANE Database?
The Cleft Registry and Audit NEtwork (CRANE) database is a national clinical registry that has collected information about all children born with cleft lip and/or cleft palate in England, Wales and Northern Ireland since 2000, when the database was set up by the Department of Health*.
We now have records for 21,865 children born with a cleft in this registry. Sections 4 and 5 summarises key registry information for children born between January 2017 and December 2019.
Typically, children with a cleft lip and/or palate need cleft team care from birth to adulthood. This is why it is important to record information on these children at birth or at diagnosis, and into childhood to inform their care.
CRANE is also a national clinical audit. An audit in healthcare is used to improve the care of patients. CRANE is committed to helping professionals provide the best evidence-based cleft care through the information we make available in our reports. Section 6 summarises key audit information for 5-year-old children born between January 2011 and December 2013.
With the informed consent of parents/carers, CRANE collects information and reports on the following for children with a cleft:
- The care they have received, and
- how well they are getting on in terms of their overall growth, speech, dental health, facial growth, and psychological wellbeing.
We do not use any information in our reports that could identify patients or their families.
For more information on why CRANE collects this information and how the information is handled, please read our CRANE Database Information Leaflet.
*CRANE is overseen and guided by the Cleft Development Group – see the Glossary for more information on this.
What other information does CRANE collect and use?
With parent’s/carers’ consent, CRANE follows the health of children with a cleft by linking to their official records held by the health system.
This is called data linkage. It gives CRANE more information about the treatments that children with a cleft receive, as well as the outcomes of these treatments.
- This information is difficult to record by asking parents/carers directly or at a clinic, as this may not be easy to remember in detail. For example, the precise dates of each of their child’s surgical treatments.
- Allowing CRANE to link to this information in children’s official records is voluntary and parents/carers and their child are free to withdraw their child’s information from the database at any time, without giving any reason, and without this affecting the treatment that they receive.
- For a full list of the official records that we currently link to and intend to link to, please read CRANE’s Privacy Policy.
No ‘data linkage’ information is collected without the consent of parents/carers. Children and their families cannot be identified from CRANE’s findings and publications.
If you want to find out more about the other sources of data already collected and stored about your child, please read our CRANE Database Linkage Leaflet.
What we know about children born in 2020 with a cleft lip and/or palate
How many babies were recorded?
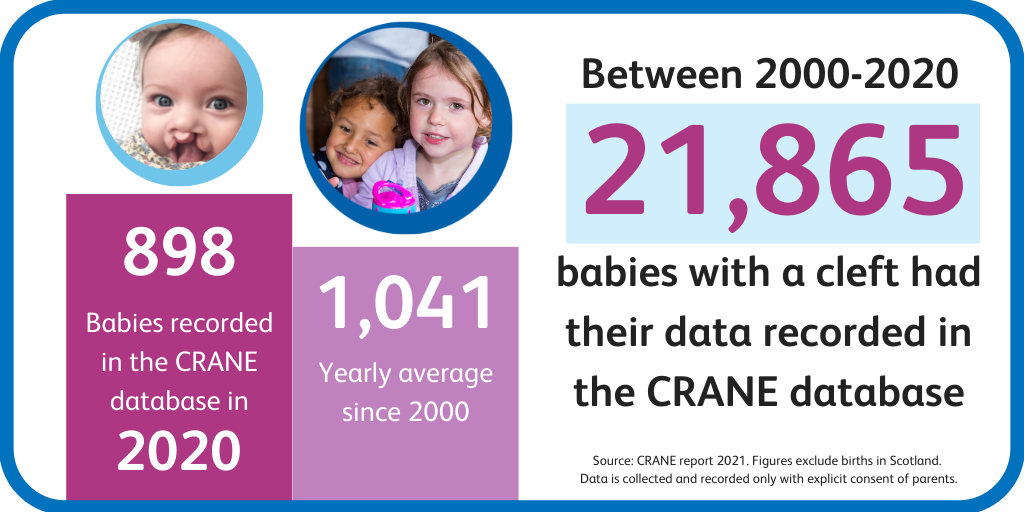
- Number of children with data recorded in the CRANE database over the last 21 years, between 1 January 2000 and 31 December 2020: 21,865
- The average number of children recorded in CRANE is 1,041 per year.
- A total of 898 children were recorded in CRANE between 1st January and 31st December 2020.
What do we know about children born between 2017 and 2019 with a cleft?
Kinds of Cleft

- Most children born in this 3-year period had a cleft palate (CP), at 44%.
- Fewer children had a cleft lip (CL, 23%), or a unilateral cleft lip and palate (UCLP, 23%). Bilateral cleft lip and palate (BCLP) was the rarest type of cleft (11%).
Collecting Consent
90% of parents/carers who had reached a decision about allowing the CRANE Database to collect data on their child, into childhood, had agreed (‘consented’) to this.
Timing of diagnosis
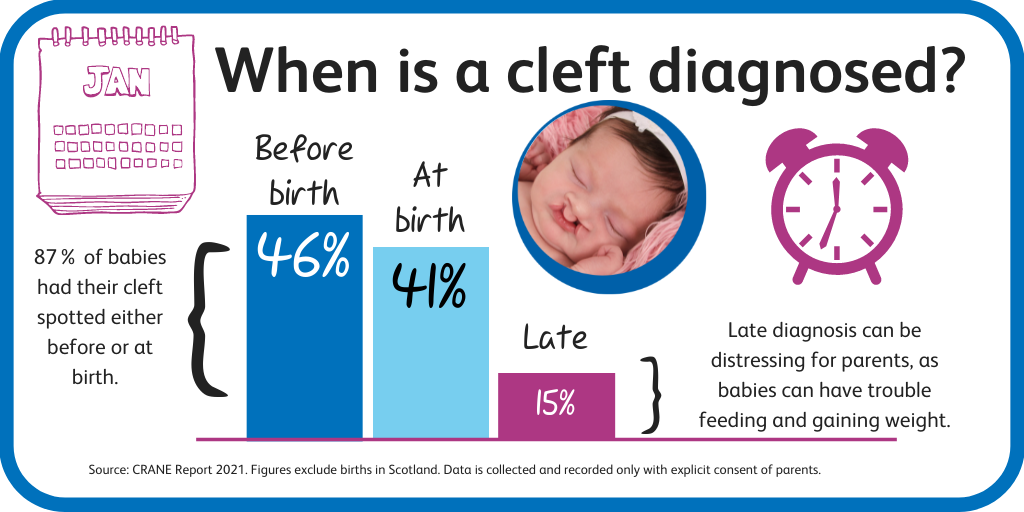
- Most babies with cleft had their condition spotted either before or at birth (accounting for 87% of diagnoses).
- 5% were diagnosed between 24-72 hours after birth, and a further 8% received a ‘late’ diagnosis after 72 hours.
- Early diagnosis is important to ensure families are appropriately supported from the earliest opportunity. Cleft palates only are rarely diagnosed prior to birth.
Who were these children?
- 56% of the babies born with a cleft were boys, and 44% were girls
What Happened After Diagnosis?
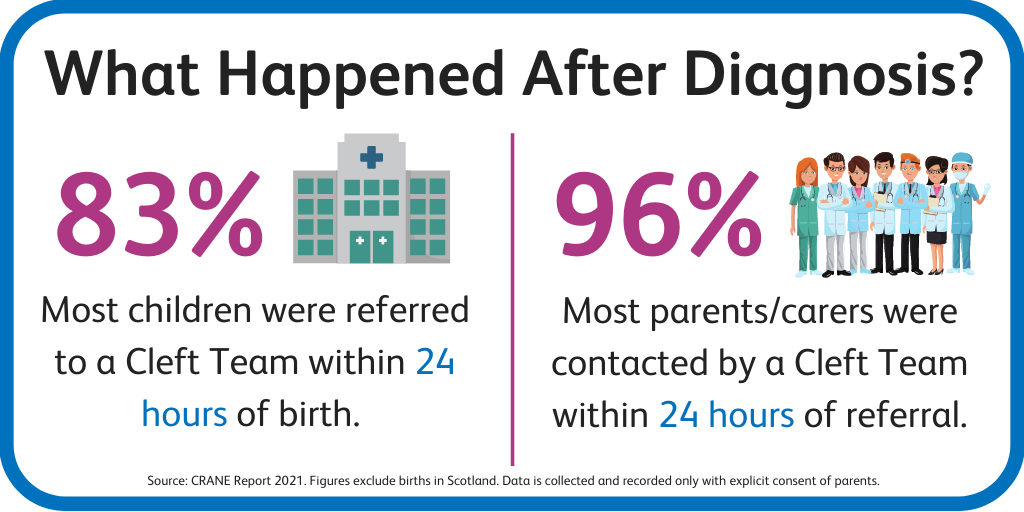
83% of children were referred by the maternity unit to a unit specialising in cleft care within 24 hours of the baby being born.
96% of parents/carers were contacted by the unit specialising in cleft care within 24 hours of referral.
What we know about 5-year-old children (born between 2011-13) with a cleft?
This section summarises information on children with a cleft at 5 years of age (born between 2011 and 2013), whose parents/carers agreed (‘consented’) to CRANE collecting information on their child’s health.

Child’s Growth
Almost nine in every ten children (87%) born with a cleft during the birth years studied had a healthy Body Mass Index (BMI). This means that most 5-year-olds born with a cleft had a healthy weight for their height (see the Glossary for more information on BMI).
Dental Health
Approximately three in every five children (62%) had no decayed, missing or filled teeth (DMFT). This is lower than the rate found in the general population (77%). This means rates of DMFT in children born with cleft lip and/or palate are higher than the general population (see the Glossary for more information on dmft).
Facial Growth
Approximately two in every five children (38%) with unilateral cleft lip and palate (UCLP) had what is known as ‘good facial growth’ when examined by orthodontists (using an assessment called the Five Year Old Index – see the Glossary for more information on the index).
This is better than the rate reported in 1998 (29%), before cleft services
were centralised.
Speech
60% of children had scores suggesting their speech was not significantly different from children of the same age born without a cleft. Children with a cleft affecting only the palate tend to have better speech than those with a cleft affecting both the palate and lip
Psychology screening
82% of children born with a cleft, and assessed with the ‘Strengths and Difficulties’ questionnaires, had scores in the low/normal range, compared to 90% of their non-cleft peers.
Psychologists offered support to the children, as needed, for the majority of children with high scores, and to 18% of those with lower scores. (see the Glossary for more information on the Strengths and Difficulties questionnaire).
What we understand from our most recent review of audit and health information

Congenital malformations in children born with a cleft
For the first time, CRANE has explored the relationship between children born with other congenital malformations and a cleft.
Establishing good links with Paediatric and Genetic services is recommended for these children.
More information about this work can be found in the research section of the annual report.
Congenital malformations of the circulatory system and speech at age 5
Children without malformations of the heart and circulatory system were more likely to achieve a speech outcome comparable to their peers at age 5 than those with these malformations**.
We recommend reporting the speech outcomes of this group of children separately.
**Based on information about children born between 2006 and 2012.
Is there a difference in cleft-related speech outcomes between girls and boys at age 5?
Females with cleft palate (with or without a cleft lip) achieved significantly better speech outcomes at age 5 than males.
This was still significant when we adjusted for different cleft types**.
This information can be used to inform service delivery.
The child’s sex should be factored into risk adjustment models when reporting cleft-related speech outcomes at 5 years.
**Based on information about children born between 2006 and 2014.
Timely diagnosis of cleft palates
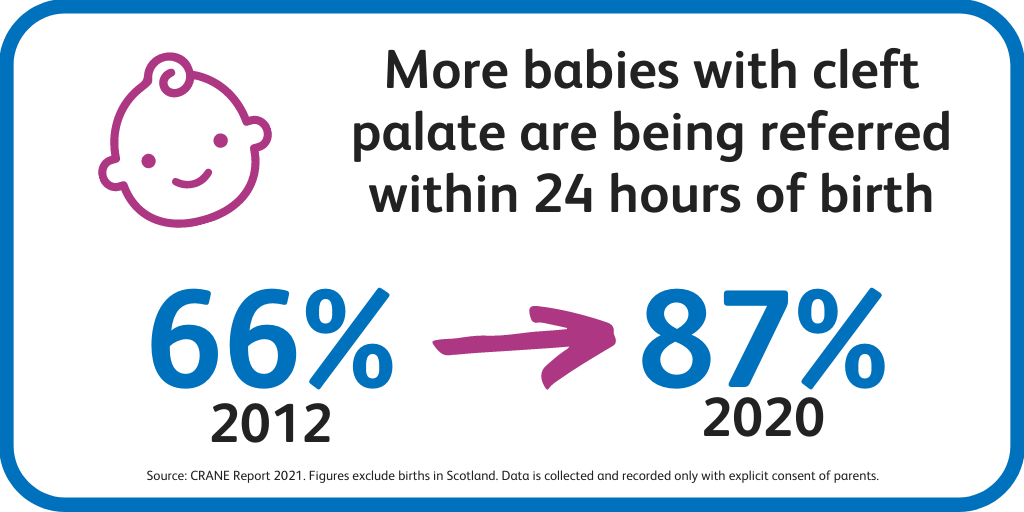
National standards state that clefts should be diagnosed within 24 hours of birth to enable immediate referral to a specialist hospital. Among children born with a cleft palate, the percentage of children referred to a cleft team within 24 hours rose from 66% in 2012 to 87% in 2020, showing improvement in immediate referral to a specialist hospital**.
This significant improvement in the timely detection of cleft palates has been particularly marked in the last five years since the Royal College of Paediatrics and Child Health (RCPCH) — in collaboration with key partners including the CRANE Database team — published a best practice guide to help healthcare professionals identify cleft palate in newborns in 2015.
- This NICE accredited guide gives recommendations to ensure early detection of a cleft palate, and to improve and standardise the way the palate is routinely examined at birth.
- A parent/carer guide is also available.
- This best practice guidance, and the RCPCH training module to reduce delays in detection of cleft palates launched in 2019, came about as a response to the CRANE reporting in 2012 that almost a third of babies with cleft palate had their condition missed at birth.
CRANE will continue to monitor rates of diagnoses of cleft palate, and work collaboratively, to further identify ways of improving the timely diagnosis of cleft palates within 24 hours of birth.
**Based on information about children born between 2012 and 2020.
How can I find out more?
If you have any other questions about the CRANE Database that are not answered by our information leaflet, you can get more information by:
- Talking to a member of your local Cleft Team;
- contacting us directly by phone on 020 7869 6610 or by email at [email protected];
- looking at the CRANE Annual Reports – available on the Reports page; and
- contacting the Cleft Lip and Palate Association (CLAPA) directly on 020 7833 4883 or by email at [email protected].
Glossary
| Body Mass Index (BMI) |
The Body Mass Index (BMI) is a widely accepted measure of weight according to height, calculated using weight in kilograms divided by the height in metres squared (kg/m2), as per the definition of BMI by the Royal College of Paediatrics and Child Health (RCPCH). BMI was estimated for all consented children registered in CRANE with a recorded height (m) and weight (Kg) at five years. These estimates were then classified into the BMI categories of underweight, normal, overweight or obese; according to the RCPCH. |
| Cleft Development Group (CDG) |
NHS group representing all stakeholders in cleft care (including the Cleft Lip & Palate Association (CLAPA)). The CDG is responsible for providing data for cleft births and cleft treatment for England and Wales and it endeavours, with the cooperation of the health services in Scotland and Northern Ireland, to do so for the whole of the UK. If you want to find out more about the CDG, please visit the Cleft Development Group page on the CRANE website. |
| Cleft Lip | A condition that creates an opening in the upper lip between the mouth and nose. It looks as though there is a gap in the lip. It can range from a slight notch in the coloured portion of the lip to complete separation in one or both sides of the lip extending up and into the nose. A cleft on one side is called a unilateral cleft. If a cleft occurs on both sides it is called a bilateral cleft. A cleft in the gum may occur in association with a cleft lip. This may range from a small notch in the gum to a complete division of the gum into separate parts. |
| Cleft Lip & Palate Association (CLAPA) | The only UK-wide voluntary organisation specifically helping those with, and affected by, cleft lip and palate. Find out more about CLAPA. |
| Cleft Palate | This occurs when the roof of the mouth has not joined completely. The back of the palate (towards the throat) is called the soft palate and the front (towards the mouth) is known as the hard palate. If you feel the inside of your mouth with your tongue, you will be able to notice the difference between the soft and the hard palate. A cleft palate can range from just an opening at the back of the soft palate to a nearly complete separation of the roof of the mouth (soft and hard palate). |
| Decayed, missing or filled teeth (dmft) | This is a measure of oral health and describes the total amount of tooth decay / dental decay or cavities in children – specifically the total number of teeth or surfaces that are decayed (d), missing ((m), which includes teeth that do not develop and those removed due to dental disease), or filled (f). Children’s scores can range from 0 to 20 for affected teeth and 0 to 88 for affected surfaces. |
| Five-Year-Old Index | An assessment used to examine dental models of the teeth with five-year-old children with a Unilateral Cleft Lip and Palate (UCLP). The index evaluates the effects of children’s main surgery on their facial growth before any other interventions, such as orthodontics or alveolar bone grafting, which may influence this growth further. Patients categorised as ‘1’ and ‘2’ on the index are considered to have the best possible outcomes, while those categorised as ‘4’ and ‘5’ are thought to have the worst outcomes in terms of facial growth (the upper jaw has not grown as far forward as the lower jaw generally), and they may benefit from further surgery to correct this once facial growth is complete. |
| Psychosocial health | Health and well-being based on the combination of both a person’s thoughts and behaviours (the psychological part) and a person’s social environment (the social part). |
| Strengths and Difficulties Questionnaire | An emotional and behavioural screening questionnaire for children and young people (both with and without conditions like cleft) used by psychologists to guide the care they provide to them. It asks about 25 attributes (e.g. how they interact with other children), and allows psychologists to understand whether children’s symptoms or behaviours are close to average, slightly raised, high or very high. A higher score indicates a child may need more support in certain areas. |