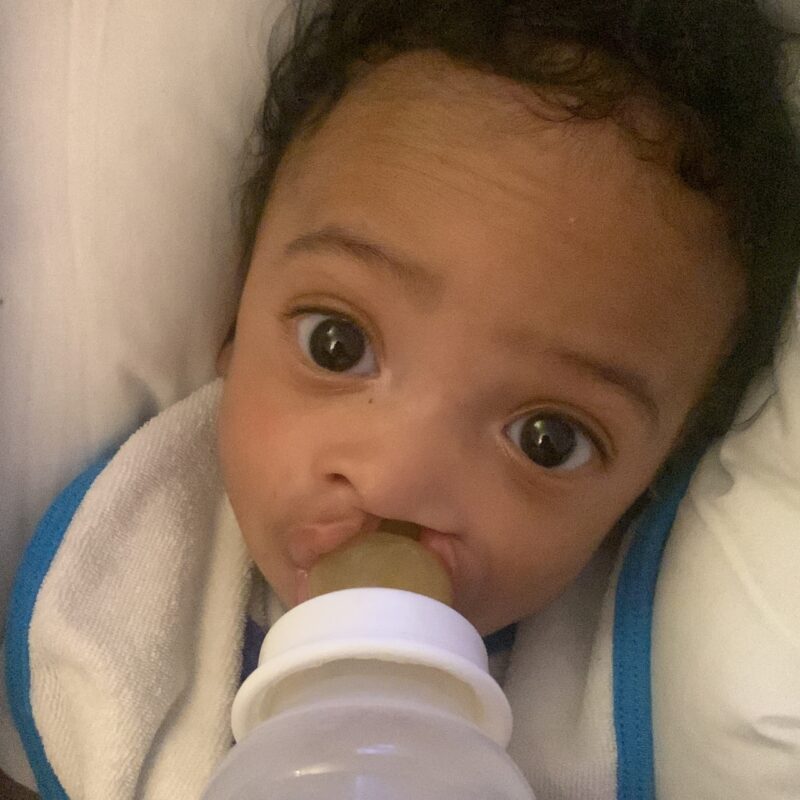
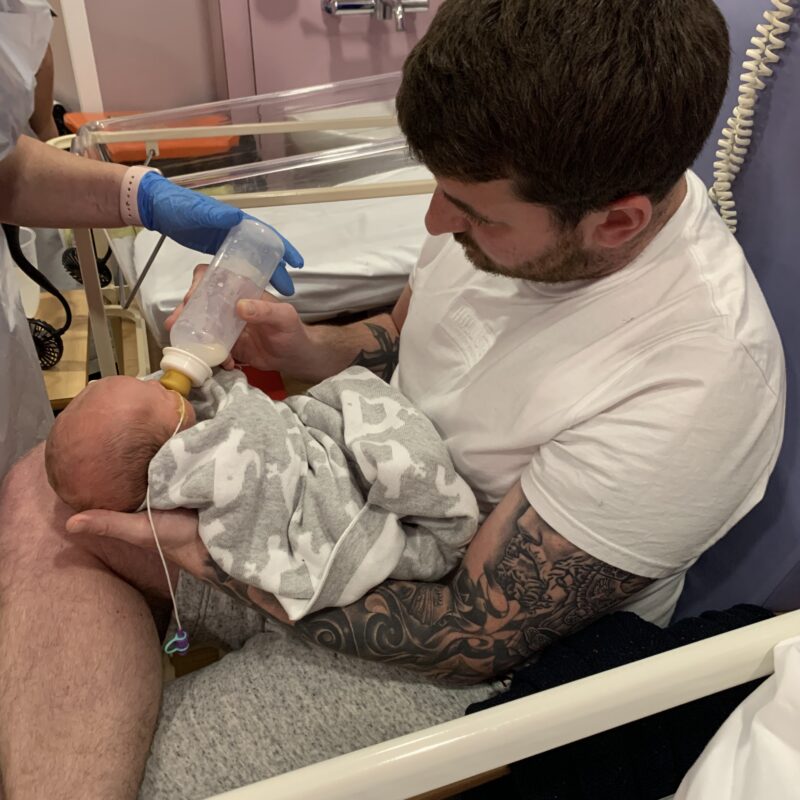
This page explains the common issues you may face when feeding a baby with a cleft and shares some common solutions.
The information here is a general guide only and should never replace the advice given to you by medical professionals. You should talk to your Cleft Nurse Specialist if you have any specific questions or concerns about feeding your baby.
Common issues when feeding a baby with a cleft
Coping with feeding issues can be stressful, so it’s important to look after yourself as best you can and seek out support when you need it. You do not have to go through any of this alone.
To feed, babies create a ‘vacuum’ with their mouth, much like we do when drinking through a straw. We do this by creating a tight seal with the lips and closing the back of the mouth off from the nose using the soft palate (the roof of the mouth towards the back of the throat).
If a baby has a cleft palate, they may not be able to close off the back of their mouth from their nose to create this vacuum. It’s like if you tried to drink through a straw which had extra holes in it – even if you managed to get some of the liquid into your mouth, it would take much longer and be more tiring.
If a baby has a cleft lip, the shape and size of their cleft might make it harder for them to create a tight seal around the breast or bottle, leading to the same issues.
What can help?
Your Cleft Nurse Specialist will assess your baby’s feeding needs shortly after birth.
They may recommend using specialist bottles available from CLAPA to either replace or supplement other feeding methods. These special bottles allow babies to feed without the need for them to create a vacuum with their mouths.
In some cases, babies may need to use a nasogastric (NG) tube to ensure they feed enough. This is a small tube which goes through the nose or mouth and into the stomach. It is usually used alongside breast or bottle feeding.
Because babies born with a cleft might not be able to create a vacuum with their mouths, they may swallow more air when feeding, especially if the flow of milk is either too slow or too fast.
Signs a baby is swallowing too much air when feeding can include having a blue ‘moustache’, being extra sleepy, or bringing up some of their feed. You might also hear a ‘hissing’ sound during feeding.
What can help?
If this happens often, try stopping a few extra times during the feed to burp your baby.
You can also talk to your Cleft Nurse Specialist about trying other bottles or teats, or making sure you’re using the bottles and teats correctly.
As well as creating a vacuum with their mouths, babies need to have their tongue in the right place to be able to draw milk out of a nipple or teat. Your Cleft Nurse Specialist will show you how to make sure your baby’s tongue is in the right position when they show you how to feed your baby.
Babies born with Pierre Robin Sequence (PRS), a condition with several symptoms including a cleft palate, have a smaller lower jaw (mandible). In their first 3-5 months of life, their tongue is positioned at the back of the mouth, which can affect breathing and swallowing. If your baby has PRS, you will be given specialist advice on how to manage their feeding needs.
A cleft palate can mean milk gets into the nose during feeds, especially if the flow of milk is too fast.
Babies might also sneeze out milk, or milk may come through their nose when they’re being sick.
Breast milk doesn’t irritate the delicate tissue here, but formula milk can leave deposits which could make your baby congested.
What can help?
Babies don’t produce much saliva during their first two months of life, so they might not be able to clear these deposits out on their own.
If your baby drinks formula milk, giving them 2-3 teaspoons of cooled boiled water after a feed can help to clear out any milk from their nose.
As they get older, they will usually be able to clear out any milk on their own, but you’ll want to have extra cloths and bibs handy.
All babies can lose a little weight after birth, but usually regain it in two to three weeks. If your baby is having five to six wet nappies a day and regular motions, and is generally healthy and alert, they are likely getting enough milk.
Because it can be more difficult to feed a baby born with a cleft, your baby may struggle to feed enough and gain weight.
What can help?
Talk to your Cleft Nurse Specialist or your GP if you are at all concerned about this.
Sometimes, babies need to be given special high calorie milk to help them take in enough nutrition in their early weeks.

Easing the first few hours: Feeding
Weaning babies born with a cleft
If your baby has a cleft palate, food may get into (or come out of!) their nose while they eat. They may even sneeze to get the food out.
This might be distressing at first but is nothing to worry about, and your baby will soon learn to cope. Just make sure you finish mealtimes with a drink of water to help clear out any food from the nose and cleft area.
It might be hard for babies with a cleft palate to drink from ‘non-spill’ beakers or sippy cups, as they’ll run into the same issues when trying to create a vacuum with their mouths.
A ‘doidy cup’ is often recommended for babies and children who struggle to suck through a teat or spout, but as these have an open top, they’re usually better for older children.
After a cleft palate repair operation, your Cleft Team might recommend you use a sippy cup with a soft or short spout which has less chance of disturbing the surgical site.
If a cleft affects the gums, the position of teeth can make them difficult to clean, leading to tooth decay and other problems.
You can help to keep your child’s teeth clean by limiting sugar, avoiding sweet drinks, and giving sugar-free medicine and vitamin supplements at mealtimes.
Babies using bottles and teats from CLAPA
Bottle feeding a baby born with a cleft
CLAPA supplies special bottles and teats which have been designed for babies born with a cleft.
Not all babies born with a cleft will need to use these. For those that do, they can help to make sure babies get the nutrition they need in a reasonable amount of time.
Some of these bottles work by gently squeezing the milk into the mouth while the baby suckles. Others use a special valve to express milk while a baby works at the teat with their tongue. In both cases, they’re designed to allow a baby to feed without them needing to form a vacuum with their mouths.
Tips for bottle feeding babies born with a cleft
-
Talk to your Cleft Nurse
Your Cleft Nurse Specialist will make sure you are confident about feeding your baby before you go home from the hospital. You should contact them directly if you have any questions or concerns about feeding your baby. CLAPA staff are not medically trained and cannot give advice on using the special bottles and teats we supply.
-
Make sure they have a tight seal around the teat
A baby needs to form a tight seal with their lips around the teat to be able to bottle feed effectively. Orthodontic teats (like the MAM teats supplied by CLAPA) can help to fill the gap left by a cleft lip and help a baby to feed without swallowing too much air.
-
You may need to try different bottles and teats
If your baby is feeding slowly or swallowing too much air, talk to your Cleft Nurse Specialist about trying different teats. You may need to go up a size or try a different shape.
-
Find the right position
Most of the time, you’ll be able to nurse your baby in the normal ‘cradling’ position. Some babies may need to be fed in a different position, such as on their sides. Your Cleft Nurse Specialist will explain this to you.
-
Check your bottles fit your steriliser
If you get an electric sterilising machine, make sure it fits your chosen bottles and teats. Both the MAM and Dr Browns bottles are longer and thinner than some commonly used bottles in the UK.
-
Use cold water sterilising
The special bottles and teats supplied by CLAPA are made of materials which can break down faster if they are regularly sterilised with steam or are left soaking for a long time. Cold water sterilising methods can help these bottles and teats to last longer.
-
Don't use soft bottles without training
When using soft bottles (like the MAM bottles supplied by CLAPA), these need to be gently squeezed while your baby is sucking to help the flow of milk. Squeezing the bottle when your baby is ‘resting’ during feeds and not sucking can cause them to choke or cough. This is why it’s important to only use these bottles if you’ve been shown how by a trained medical professional.
Tips on expressing breast milk
Expressing milk involves using a breast pump to stimulate milk production and then feeding your baby using a bottle.
Talk to your Cleft Nurse Specialist or midwife about expressing milk. Your Cleft Team or a local organisation may be able to lend you a breast pump.
Tips from other parents and carers
- Get an electric breast pump if possible. The manual pumps are handy for when you’re on the go, but they can be time-consuming and tiring.
- Use syringes to manually express colostrum before your milk comes in. Your local chemist can point you in the right direction.
- Breast milk bags are great for storing your milk in the freezer. Some brands come pre-sterilised, are double layered for better long-term storage, and are compact so they take up less space.
- A large plastic box filled with tap water and steriliser tablets is ideal for cleaning all the smaller removable accessories from the breast pump.
- Hands-free expressing bras leave you free to multitask!
Tips on formula feeding
You may choose to give your baby formula milk, or a mixture of expressed breast milk and formula milk.
Tips from other parents and carers
- Get plastic water holders (ideally BPA free) to store pre-boiled water so you don’t have to worry about these when making bottles in the middle of the night.
- Formula powder is the most economical option and great for everyday use, but formula cartons can be very helpful in the early days and weeks when you’re still getting into your routine.
- A formula powder dispenser is very helpful when out and about, or when preparing a quick bottle at home. They’re also great when you need to hygienically transport powder formula away from home.
Breastfeeding a baby born with a cleft
A cleft can make breastfeeding extremely difficult. Your Cleft Nurse Specialist will carry out a feeding assessment shortly after your baby is born to explore all the options with you and give advice on how you can safely and effectively feed your baby.
Even if you can’t breastfeed as you may have hoped to, any amount of breastmilk is still beneficial. You may still be able to express milk and bottle-feed your baby, either exclusively or supplemented by formula milk.
A good flow of milk from the breast will help with whatever method you choose. Talk to your midwife or a feeding specialist about how to encourage this by massaging the breast, using a breast pump, or hand expressing.
It is important to remember that many babies struggle to breastfeed even without a cleft. You do not have to deal with any difficult feelings you may be having alone. Please reach out for support if you need it.
Babies with a cleft lip (without a cleft palate) may be able to breastfeed, but it depends on the shape of the cleft in their lip and whether the breast can ‘mould’ to the gap.
A hissing sound during feeds usually means air is coming into the mouth, so you may need to try another position to help your baby to form a tight seal.
The nipple needs to stay on the back of their tongue, so you may need to help your baby by holding the breast in the mouth, as the nipple might move towards the front of their mouth as they feed.
You will likely need to try several different positions and methods over time before you find one which works. Talk to your Cleft Nurse Specialist for expert advice on this.
Breastfeeding a baby born with a cleft palate may be possible when the cleft is very small or narrow.
The breast needs to be held well into the area where the palate is intact so that the baby can get a good grip and work at the breast with the tongue. A baby born with a cleft palate will need help in achieving a good ‘latch on’. A Cleft Nurse Specialist may be able to help you with this.
If your baby can’t suckle from the breast, they may still be able to still lick milk expressed onto the nipple.
Any amount of breastmilk is still beneficial, so you may wish to try expressing your milk and using specialist bottles and teats to replace or supplement breastfeeding.
Feeding your baby after a cleft repair operation
After a cleft lip repair operation, you can usually start feeding your baby again using your usual feeding methods right away.
They may recommend you avoid dummies or comforters while a lip repair is healing.
In some cases, your surgeon will recommend you use a ‘cup and spoon’ method for a short while.
The advice you will get will depend on how old your baby is when they have their palate repair operation and whether they are still using a bottle for milk or other drinks.
It’s a good idea to ask your Cleft Team about this before the operation, as they might recommend you avoid using a bottle for a short time while your baby is healing. If this is the case, you may want to get your baby used to using a spoon bottle or a sippy cup with a short spout before their operation so they find it easier to use afterwards.
They might also advise you to avoid dummies while your baby’s palate is healing.
Find support for you and your family
Antenatal Support Groups
CLAPA’s regular Antenatal Support Group events are a chance for new and expectant parents to create a support network, ask questions and share your concerns. You are not alone.
Read stories about feeding
Many parents of children with a cleft have written about their experiences of feeding their babies. They have shared these personal moments, from the hopeless to the triumphant, to help new and expectant parents prepare for their baby’s future.
Talk to another parent
Parent Supporters are trained by CLAPA to support others one-on-one, either over the phone or through email. They understand just what you’re going through, as they’ve been through it all themselves!
Support on social media
CLAPA has a private support group on Facebook with over 10,000 UK parents and carers of children born with a cleft.
Counselling
CLAPA offers a dedicated counselling service for parents and family members (18+) of children born with a cleft.
Psychological support from your Cleft Team
The Clinical Psychology Team with your Cleft Team can help you to talk through any difficult feelings you might be having around feeding your baby. Talk to them about making an appointment.
Read stories from other parents and carers

Oakley’s cleft palate saves his life
Two-year-old Oakley has Apert Syndrome, a rare genetic condition that causes fusion of the skull, hands and feet bones. He was also born with a large cleft palate, which saved his life when his other airways became obstructed.

Baby Finn’s moment of fame in advertising campaign
Next time you’re out shopping look up at the video boards and you might just see one of our CLAPA community babies advertising Pampers nappies.

Happy Grandparents’ Day
In celebration of all our wonderful CLAPA grandparents we spoke to Audrey and Dave about their cleft journey with granddaughter Rebecca.