Media Guidelines
This page explains what a cleft lip and palate is, the impact it can have on families and individuals, and what CLAPA does as a charity.
Download ‘Notes for Editors’ (PDF)
- How does it happen?
- What is the impact of a cleft lip and palate?
- How is it treated?
- Terms and language
- Writing about people affected by cleft
About Cleft Lip and Palate
In early pregnancy, the different parts of the face form separately and then join together. For one in 700 babies, the different parts don’t fully join, resulting in a gap or ‘cleft’ in the upper lip or the roof of the mouth.
Every day in the UK, three babies are born with a cleft. It can have an ongoing impact on feeding, speech, hearing, teeth placement and more. The treatment pathway is 20+ years, and many babies have their first surgery at just three months old.
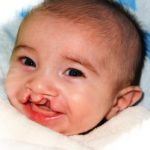
A ‘cleft lip’ is one or two notches or gaps in the upper lip which can range from a small notch in the coloured part of the lip to wide gaps that extend up into the nostrils. A ‘cleft palate’ is a gap in the roof of the mouth. Babies can be born with a cleft lip, a cleft palate, or both together.
1 in 700 babies are born with a cleft across the world. That’s three every day in the UK.
How does it happen?
In most cases, it’s the result of many different genetic and environmental factors coming together in a way that can’t be predicted or prevented. It can happen in any pregnancy, even with no family history.
It is very unlikely that a child’s cleft developed because of something the parents did or didn’t do. In some cases, a cleft is caused by a syndrome such as Pierre Robin Sequence or Stickler Syndrome, and these will have their own causes and outcomes.
Because there are so many complex factors that can lead to a cleft, it’s unlikely there will ever be a ‘cure’ that will stop it from happening. This is why CLAPA focuses on improving the lives of people born with a cleft and supporting their families.
What is the impact of a cleft lip and palate?
Surgeries: Starting at just three months old, people born with a cleft will need one or more surgeries to close the gap(s) and help with any ongoing issues. Some will have more than 20 surgeries by the time they reach adulthood.
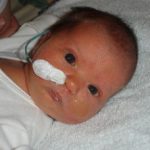
Feeding: Babies born with a cleft often can’t form a vacuum with their mouths; it’s like trying to suck through a straw with a hole poked in it. This means they can’t feed from a breast or regular bottle. CLAPA is the only UK supplier of specialist bottles and teats for babies born with a cleft. These bottles and teats are used and recommended by NHS Cleft Nurse Specialists. Some babies will need a nasogastric tube which runs from their nose to their stomach.
Hearing: Children with a cleft palate are more likely to develop glue ear and associated ongoing hearing issues. Many children with a cleft palate need grommets or hearing aids.
Speech: A cleft palate means extra air can escape through the nose while speaking, causing speech to sound nasal or muffled. Half of all children with a cleft palate need ongoing speech therapy to help with this. By age 5, around 40% of these children will still have noticeable speech differences.
Teeth placement: Children with a cleft affecting their gum will need orthodontic work, which can be quite extensive. This usually includes a bone graft surgery at 7-12 years old, which helps teeth grow in the gap in the gum. Children with a cleft are also more susceptible to tooth decay and other oral health issues, which can extend well into adulthood.
Facial growth: In some cases, a cleft lip can cause a child to grow up with a ‘flat’ profile or an underbite. In some cases, further surgery will be offered to help with both functional and cosmetic concerns.
Educational Achievement: Cleft is not linked to learning difficulties, but children with a cleft tend to have lower educational attainment levels. Research says there’s no obvious medical reason for this, which suggests it’s likely because of a lack of school support for hearing, speech, and other issues that may limit a child’s engagement in education.
Emotional wellbeing: A cleft often means a child will grow up looking or sounding different to their peers and having multiple hospital appointments, including surgeries. Coping with staring, comments, bullying, and discrimination can impact emotional wellbeing and self-esteem.
How is it treated?
Cleft has a 20-year treatment pathway handled from the point of diagnosis by one of the multidisciplinary NHS Cleft Teams around the UK.
A cleft lip is surgically repaired when a child is 3-6 months old. A cleft palate is usually repaired between 6-12 months. Every child’s cleft is unique, as are their treatment needs.
Treatment may include further surgeries to help with speech, hearing, teeth placement, and changing the appearance of the face and profile. Some of these are major surgical procedures requiring years of preparation and a lengthy recovery time. Hearing aids or grommets are commonly used to help with hearing in children with a cleft palate, and around half will also undergo speech therapy.
CLAPA provides non-medical support beyond the hospital walls. The charity’s work aims to bring people affected by cleft together to support each other, build knowledge and confidence to help them take an active role in their cleft care, and feel more positive about the future.
WRITING ABOUT CLEFT
Terms and Language
Cleft lip is one or more gaps in the upper lip. Cleft palate is a gap in the roof of the mouth. Someone can be born with a cleft lip, a cleft palate, or both. These terms should not be used interchangeably.
‘Cleft palate’ is often incorrectly used to mean ‘cleft lip’ or ‘cleft’ as a condition. Please check these diagrams to make sure you’re using the right terms.
We refer to cleft and types of cleft as singular, so “people born with a cleft palate” rather than “cleft palates” or “clefts“.
The term ‘harelip’ (or ‘hairlip’) is outdated and offensive; it should not be used. Some adults may have had their treatment at a time when this was still the medically accepted term, and when an adult uses this term to describe their own experiences, CLAPA does not ‘correct’ its use.
Cleft is a condition, not an illness, sickness or disease.
Under the Equality Act 2010, a cleft by itself is not considered a disability. However, each case is unique. A cleft could affect someone’s speech, hearing, eating or self-esteem in a way which is significant and long-term enough that this would be considered a disability.
‘Disfigurement’ has a legally protected meaning, but CLAPA prefers not to use it when talking about cleft in general due to its negative connotations. For the same reason, we also do not use the terms ‘birth defect’ or ‘deformity’. We prefer ‘condition’, ‘visible difference’, or a description of what a cleft is (see above).
We avoid words like ‘improve’, ‘fix’, ‘problems’, or ‘normal/abnormal’, as these are value judgements which make assumptions about how people may think of their cleft. We prefer more neutral terms like ‘affects’, ‘change’ or ‘difference’, e.g. ‘A cleft can affect teeth’, ‘surgery to change the shape of the nose’, or ‘Jane’s cleft palate means her speech sounds different to other children’.
Writing about people affected by cleft
CLAPA uses ‘People First Language’ when talking about anyone with a cleft. This means we mention the individual before we mention the condition, e.g. ‘baby with a cleft’ instead of ‘cleft baby’.
When describing people born with a cleft, use neutral, objective language which acknowledges a difference without placing a value judgement on this difference, assuming the impact it has on the individual, or implying it’s the fault of the individual or their parents.
Try not to sensationalise cleft or the ways in which it may affect someone’s life, and take care to humanise the subjects of any articles to evoke empathy rather than pity. Most people will empathise with (for example) a mother worrying about her young baby having surgery, and we believe it’s important to focus on these shared emotions and experiences when telling a story rather than ‘othering’ someone because of a condition like cleft.
Avoid overly patronising phrases about how someone’s personality or another quality is more important than their appearance (e.g. “It’s what’s on the inside that counts”), as this is typically uncalled for and assumptive of an individual’s values and views of cleft.
Never suggest that the audience’s inaction will cause harm to a particular individual (e.g. “Without your help, Tom’s online support group will end, and he will have no one to talk to.”).
Readers should never be asked to express an opinion on someone’s appearance (e.g. “Like this post if you think Jane is beautiful regardless of her cleft”), and a particular person born with a cleft should never be used to ‘prove a point’ (e.g. “The media doesn’t believe people with scars are beautiful, but look at Jane”).
ABOUT CLAPA
The Cleft Lip and Palate Association (CLAPA) is the only national charity supporting people affected by cleft lip and palate in the United Kingdom.
The charity brings together people affected by cleft to help them connect with others who share their experiences, welcoming them into a supportive community for life. CLAPA’s purpose is to make sure no one affected by cleft in the UK goes through their journey alone.
CLAPA works closely with NHS Cleft Teams, but we are entirely independent and receive no NHS or government funding. We rely on fundraising and donations from the public and grant-making organisations to continue our work.
Our Work:
- Online support groups and events help people to connect with others, share their experiences and hear from others at all stages of the cleft journey
- Trained volunteers give one-to-one support and reassure those most in need that they can cope with whatever lies ahead
- Babies born with a cleft often need special bottles and teats to feed, and CLAPA produces and provides these to hundreds of new families every year
- Services for under-18s help them to build confidence and feel in control of their care, including ‘Camp CLAPA’ adventure weekends and a mentoring programme
- Adult Services connect adults born with a cleft to others with shared experiences and ensure they can access the care and support they need
- Working closely with the nine specialist NHS Cleft Teams in the UK to improve care and support patients and families with accessing treatment
- Supporting people affected by cleft to get involved with research projects
CLAPA’s History
CLAPA’s Services
CLAPA’s Charity Commission Listing
CONTACT DETAILS
For general media enquiries, please contact Anna Martindale (Head of Impact) at [email protected]
When time allows, we would happily act as a sensitivity reader to ensure the correct terms are used.
MORE RESOURCES
Face Equality International has produced an International Media Standard on Disfigurement, which CLAPA fully supports.